What is a Nurse Practitioner?

Nurse practitioners (NPs) are registered nurses with advanced training to deliver high-quality, patient-focused care in diverse healthcare settings. In the changing healthcare landscape, strengthening NPs’ scope of practice and contributions is crucial to acknowledging their importance in the medical profession. At DNP Nursing Project Help, we help nurse practitioners throughout their study and practice, starting from school selection and document preparation, to coursework, by writing tasks such as capstone projects, dissertations, essays, among others. This article contains a description of what nurse practitioner is, a discussion on education and certification requirements, scope of practice, types, comparison with other healthcare professionals, their advantages in healthcare, limitations and challenges, global perspective, and the future of NPs.
Nurse Practitioner Definition and Roles
An NP is a registered nurse (RN) who holds a graduate-level degree, often a Master of Science in Nursing (MSN) or Doctor of Nursing Practice (DNP), and has extensive clinical training. NPs can diagnose and treat acute and chronic conditions, prescribe medications, order and interpret diagnostic tests, and carry out preventative care. Most U.S. states and numerous countries permit NPs to independently practice or work jointly with physicians, as allowed by regional regulations. NPs use a holistic approach involving medical know-how and prioritizing health education, illness prevention, and customized care. Our team helps scholars write nursing tasks such as dissertations, DNP projects, or university application documents, such as recommendation letters, CVs, and personal statements, at affordable rates.
Certification and Educational Requirements
NPs’ training enhances their medical knowledge and develops their leadership, critical thinking, and decision-making skills in the complex clinical environment. The advanced training of NPs equips them with the clinical judgment and expertise to handle a wide range of healthcare issues. Applicants who wish to join NP should have a BSN or equivalent degree and earn a graduate degree, MSN or DNP in a specific area of population focus.

Scope of Practice
NPs possess a flexible range of clinical expertise, enabling them to provide high-quality patient-centered care across various health care environments. Full practice authority states allow NPs to work without the supervision of physicians, acting as primary care providers. NPs’ scope of practice generally encompasses:
- Conducting thorough patient assessments.
- Diagnoses of medical conditions.
- Planning and implementing treatment programs.
- Prescriptive authority, such as controlled substance prescriptions (in most states).
- Prescription and interpretation of laboratory and imaging tests.
- Offering health education and coaching.
- Integrating care with other healthcare providers.
Types of NPs
NPs specialize in particular population groups or medical fields. NPs’ specialties allow the professionals to deliver focused and quality care that meets the individual needs of their patients. Key specializations in NP are:
1. Family NP (FNP)
FNPs are primary care providers to individuals throughout the lifespan, including newborns, children, older adults, and individuals with various needs. FNPs focus on long-term health promotion by emphasizing preventative care, including screenings, lifestyle counselling, and vaccination. FNPs treat chronic illnesses such as diabetes, hypertension, and asthma, and can develop long-term relationships with patients and their families.
2. Adult-Gerontology NP (AGNP)
AGNPs provide healthcare services to patients of early adulthood age and geriatric patients. AGNPs deal with age-related health issues, including osteoporosis, cardiovascular diseases, and cognitive impairment, prioritizing quality of life. AGNPs practice in various environments, such as rehabilitation centers, primary care clinics, hospitals, and long-term care facilities.
3. Pediatric NP (PNP)
PNPs focus on child health development, covering infancy and adulthood. Routine well-child visits, immunizations, and common childhood illness detection are all examples of preventive services that PNPs offer. PNPs also collaborate with parents and caregivers to reach developmental milestones and provide age-appropriate preventive care to children.
4. Women’s Health NP (WHNP)
WHNPs provide comprehensive care to the female reproductive system. A WHNP provides postnatal and prenatal care, birth control counselling, and menopause management. WHNPs work at obstetrics and gynecology clinics, community health centers, and women’s health advocacy programs.
5. Acute Care NP (ACNP)
ACNPs treat patients who have extreme, complex, or fast-accelerating health-related issues. ACNPs are prevalent in specialty units of hospitals, emergency departments, and ICUs. ACNPs undertake complex procedures, promptly react to patient status changes, and consult with multidisciplinary teams.
6. Psychiatric-Mental Health NP (PMHNP)
PMHNPs are professionals who engage in diagnosis, treatment, and management of mental health disorders across the lifespan of a person. PMHNPs offer psychotherapy, prescribe psychiatric drugs, and formulate individual plans. The practice setting of PMHNPs is varied as they can work in a private setting, a hospital, a community mental health center, or a correctional facility.
7. Neonatal NP (NNP)
NNPs work at neonatal care levels and deal with newborns who have acute or chronic health issues, usually in neonatal intensive care units (NICUs). NNP roles include monitoring vital signs, using life-support equipment, and managing families in stressful conditions. NNPs work with pediatric experts and neonatologists to give the best results in preterm and seriously ill newborns.
Comparison of NPs with Other Practitioners
NP vs. Physician
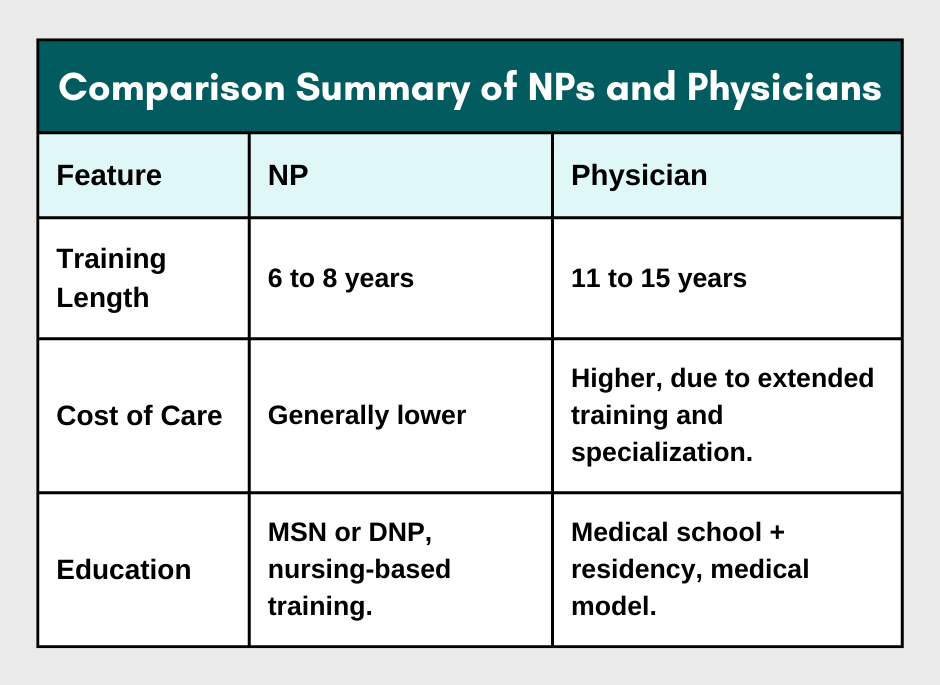

A physician completes medical school and residency, often with a broader scope in complicated or specialized care. NPs, despite their advanced skills, tend to specialize in comprehensive, preventive care, and treatment.
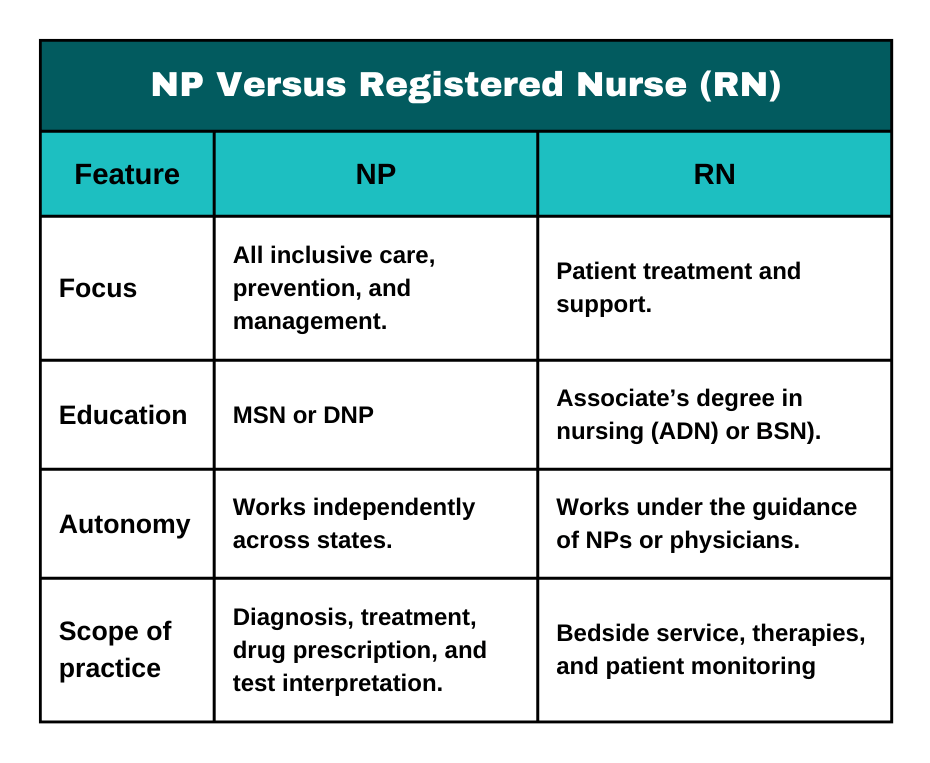
NP Versus Registered Nurse (RN)
NPs and RNs’ occupations are based on nursing skills. However, the NP is more highly educated with greater clinical authority, access to diagnose, and prescriptive authority. RNs often perform tasks in bedside care, treatments, and education of patients under the control of advanced practice providers or doctors.

NP vs. Physician Assistant (PA)
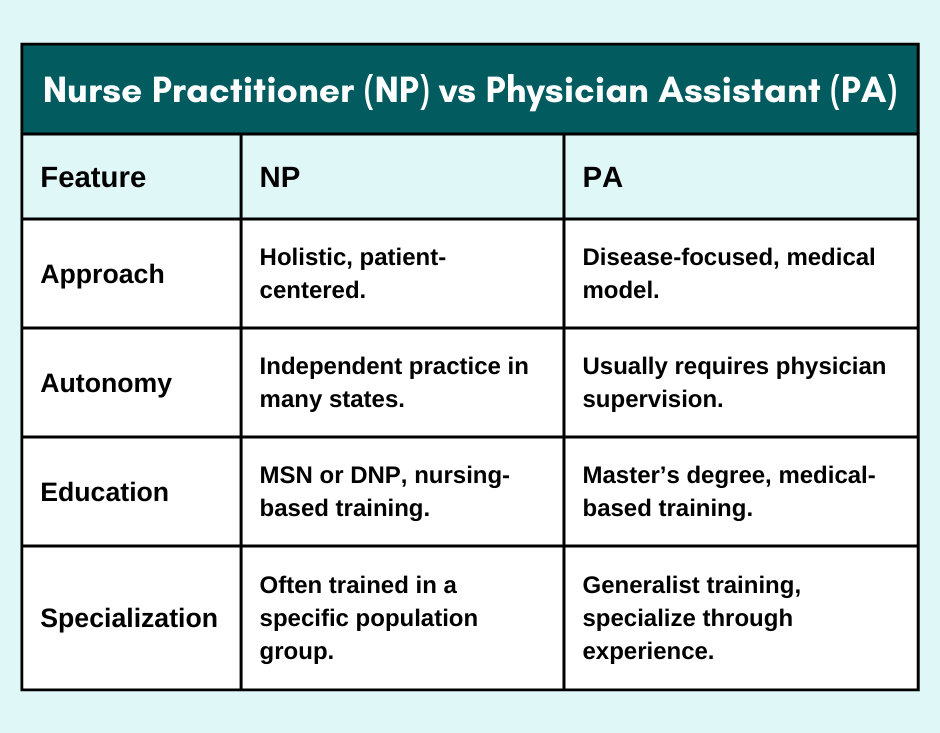
NPs and PAs are authorized to diagnose, treat, and prescribe, but have varying educational backgrounds. NPs are well-trained specialists in prevention, primary care, and patient treatment. PAs complete medical school and residency and are frequently more broadly trained in complex or focused care.
The Benefits of NPs in the Healthcare Sector
- NPs’ role is essential to increasing access to primary care, especially in rural areas and underserved communities, where physician resource scarcity is typical.
- NPs’ holistic approach targets the physical dimension of illness and the emotional, social, and environmental forces that can impact health.
- NPs also invest in patient education; consequently, people know about their conditions and treatment plans, promoting informed decision-making and care adherence. NPs specialized training equips them with clinical reasoning skills and expertise to provide a wide range of health services to patients.
- NP-led care has proven cost-effective and results in high-quality outcomes, making it a valuable asset to patients and healthcare systems.
- NPs’ significant continuity of care can lead to long-term patient-provider relationships, increase trust, enhance communication, and help manage healthcare over an extended period.
Limitations and Challenges
- The scope of practice may be heavily influenced by state rules, where certain areas wide range of health services to patients.
- The level of knowledge about the nurse practitioner role among the general population continues to be a challenge, with many patients being unaware of the scope of training and clinical authority, generating misperceptions regarding their scope of practice.
- Workforce shortages and high demand rates of nurse practitioner services can also fuel burnout and stress.
- NPs’ concerns involve sustained work to standardize practice authority across jurisdictions and increasing civic understanding of how NPs contribute to making the healthcare system so valuable.
Global Perspective on NPs
Globally, the scope of NPs differs. In nations such as Canada, the United Kingdom, and Australia, NPs are granted high authority and can deliver primary care just like physicians. Although NPs’ role is relatively established, especially in the US, the professionals’ autonomy and prescriptive authority in practice are limited when compared to physicians.
NPs are used to meet physician shortages, especially in primary care and community health. Numerous countries consider developing educational programs and legislative strategies to increase the number of NPs. This growth indicates a global trend toward using NPs to improve healthcare access, diminish wait-lists, and maximize outcomes.
The Future of Nurse Practitioner
The need for NPs is expected to increase dramatically over the next decade due to various factors transforming healthcare delivery. The increasing demand for primary and specialized services is supplemented by the aging global population with more sophisticated health needs. Meanwhile, shortages in physicians, especially those in primary care, are creating spaces where NPs can play a role in addressing urgent needs.
The US healthcare system is shifting towards preventive care and chronic disease management. In the new healthcare system, NPs will excel based on their patient-centered and holistic approach. US healthcare policy changes recognize NPs as more independent in numerous areas, allowing them to practice to their fullest education and training capacity. The emerging digital health and telehealth technologies are also expanding NP roles and equipping the professionals with skills and capabilities to serve more patients in remote locations and underserved rural environments, fostering services’ accessibility and continuity. In addition, with an average annual salary of $132,000 in the US, the NP profession attracts aspiring healthcare professionals seeking both financial stability and career fulfillment.
Summary
In the US, NPs are among the highly educated healthcare professionals whose practice spans medicine and nursing. NPs have extensive clinical skills, advanced education, and a holistic approach toward patient care that enables them to provide high-quality services that enhance accessibility, affordability, and patient outcomes. An NPs is uniquely positioned within the healthcare system when compared to RNs, physicians, and PAs, to primarily focus on comprehensive treatment, prevention, and education. NPs will be instrumental in addressing diverse populations’ needs and enhancing the quality of care globally as healthcare transforms. If you are a healthcare professional wishing to become an NP, reach out to our consultants, who will guide you through the application process to task writing. Contact us or talk to our excellent customer service agents via our live chat today for any inquiries on the nursing courses.
