Get Expert Help to Write a DNP SOAP Note

SOAP notes are used to convey information about the health status of patients as well as act as a simplified means of communication between medical practitioners. With SOAP notes, Doctor of Nursing Practice (DNP) students can simplify their note-taking processes and ensure an organized record of patients’ information to track and improve their clinical progress. For doctoral nursing scholars looking for help to write a DNP SOAP note, at DNPnursingprojecthelp, we compose excellent SOAP notes that accurately illustrate patient conditions and are personalized and specific to our clients’ needs. This article highlights some of the DNP SOAP note writing services offered by our experts, including tailored DNP SOAP note writing, paraphrasing, editing, and proofreading services.
What is a SOAP Note?
A SOAP note is a structured method of documentation used by healthcare professionals to illustrate the progress of a patient during treatment. Dr. Lawrence Weed introduced the SOAP note documentation format as part of a system of organizing the medical record called the problem-oriented medical record (POMR). Dr. Weed recommended that the client’s information be structured and organized according to a list of the patient’s problems with planned interventions for each problem, hence the development of the SOAP note. Are you looking for DNP SOAP note writing services? Get professional help with developing quality SOAP notes from our certified nursing writers and editors with guaranteed on-time delivery. We also write DNP capstone projects, discussions, data analysis, and other nursing tasks at affordable prices.
What Does SOAP Note Stand For?
The acronym SOAP represents Subjective, Objective, Assessment, and Plan. The S (Subjective) represents the patient’s signs, symptoms, family health history, frequency of the symptoms, and past illnesses. The O (Objective) contains an illustration of the data collected from the encounter with the patient. The A (Assessment) contains the health professionals’ judgment and interpretation of the statements given in the previous sections. The P (Plan) contains an illustration of what the healthcare practitioners aim to do next to meet the goals of the intervention.
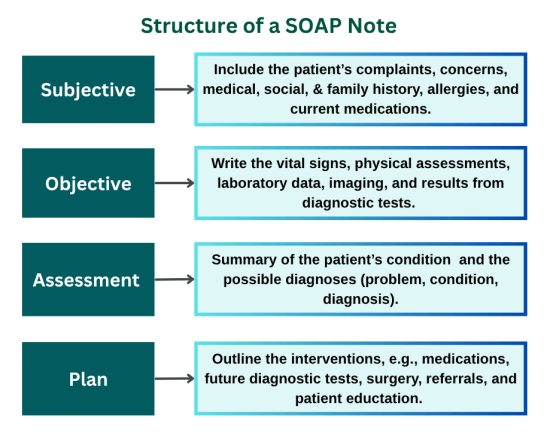
How Our Experts Structure the DNP SOAP Note
S (Subjective)
The subjective section of the SOAP note contains detailed information on the patient’s current status. Our nursing professionals develop a clinically relevant subjective narrative that reflects the patient’s perspective of their condition. When writing the subjective part of the SOAP note, we include the patient’s main complaint, detailed history of the illness, relevant history (family or allergies), review of systems, and current medications they are undertaking. By composing an outstanding subjective for the DNP SOAP note, we demonstrate the nursing scholar’s ability to prioritize patient needs and enhance quality care in a healthcare setting.
O (Objective)
The objective section contains information about all measurable and quantifiable data collected from the patient. We help DNP scholars compose an objective section that comprises physical examination and imaging results, laboratory and diagnostic data, vital signs, and a review of documentation from other medical practitioners. We develop an exceptional objective section of the DNP SOAP note using appropriate nursing terminologies to offer an unbiased and measurable record of the patient’s status.
A (Assessment)
The assessment section contains the nurse’s professional judgement of the data presented in the objectives and subjective sections. When offering DNP SOAP note writing services, we write an exceptional assessment section that illustrates any identified patterns and inconsistencies, potential limitations, comparison of progress compared to previous sessions, and the differential diagnosis. With our professional assistance, our client’s SOAP notes meet the required academic standards and demonstrate the skills and expertise required from advanced nursing practice scholars.
P (Plan)
In the plan section, the nurse determines and sets forth the specific intervention that will be used for patient treatment. In the plan section of the DNP SOAP note, our experts demonstrate the treatment that the patient will receive, the education that will be provided, and the type of specialist referrals needed. We help nursing scholars develop a well-structured plan section that demonstrates their ability to apply theoretical knowledge into practice.
Get Help to Write a DNP SOAP Note from Our Company
SOAP notes are used to provide insights into the patient’s general state and personal reports, demonstrate the observations made during sessions and evaluations, illustrate a comprehensive analysis of the patient’s condition, and contain a detailed treatment plan for the client. Our DNP SOAP writing services are designed to provide professional assistance on how to write SOAP notes for nursing students. Certified nursing writers and editors from our company help with composing various types of notes based on the client’s project, such as initial, interim, discharge, medical, and mental health.
By hiring our professional nursing experts, DNP students improve their clinical reasoning skills, a factor that is essential to advanced patient care. SOAP notes composed by our nursing experts are written in compliance with medical and nursing documentation standards, demonstrating professionalism and knowledge in the field. If you are looking for expert assistance with writing a DNP SOAP note, our professionals work within your desired timeframe to compose an outstanding SOAP note that demonstrates advanced knowledge in nursing. We also offer other nursing writing services such as DNP proposals, PowerPoints, discussions, IRB applications, and reflection papers, among others.

Hire Our Experts for the Best DNP SOAP Note Writing Services
Our company has the best writing experts who have DNP and PhD degrees in the field of nursing. Additionally, our professionals have years of experience composing SOAP notes for post-graduate nursing students. Our authors apply this experience and expertise to write quality SOAP notes, assured of approval by your supervisors.
Nursing writers from our company offer customized solutions tailored to our clients’ specific DNP programs. Some of the solutions offered by our expert writers include, but are not limited to, developing clear objective data reports, providing effective clinical assessments, and offering expert guidance on treatment care plans to implement.
Getting help to write a DNP SOAP note from our professionals guarantees our clients a quality document tailored to their specific needs. By integrating effective research resources and expert writers in the field of nursing, we compose exceptional SOAP notes that are focused and easily understood by other nurses.
Our services operate for 24 hours, enabling us to meet tight deadlines for nursing students around the globe. In case you are running on tight deadlines, hire our nursing experts today for timely delivery without compromising on quality.
Could you be looking for DNP SOAP note writing services? Look no more as we have nursing writers with over 10 years of experience writing SOAP notes tailored to our clients needs. Contact us today and leave your request for help with a SOAP note. Our friendly customer service team is available through our live chat to respond to all your inquiries promptly.
Frequently Asked Questions About Our DNP SOAP Note Writing Services
What are the Three Key Aspects of Writing a Quality SOAP Note?
SOAP notes are a crucial part of each client’s treatment. To write a quality SOAP note, first, be specific; second, avoid judgmental statements; and third, include names of other family members. Additionally, the SOAP notes should be easy to read so that information is communicated quickly to other staff members.
What are the Benefits of Using SOAP Notes?
SOAP notes enable evidence-based decision-making through documentation of the client’s progress. A major benefit of SOAP notes is that documenting patient treatment details simplifies the process of sharing information among healthcare practitioners. Other advantages include: i). It is used to track the patient’s progress, ii). helps healthcare providers to reference previous hospital sessions with the patient, and iii). enables professionalism through staying organized.
What are the Different Types of Notes in SOAP?
The types of notes in SOAP vary depending on who is writing the note. Various types include: initial, interim (progress), and discharge notes. The initial note is used in everyday clinical practice to document patient encounters. In an interim note, information obtained while reassessing the patient is included. The discharge note is similar to the interim note and is an update on the patient’s status since the last progress note was written.
How do I Get Help to Write a DNP SOAP Note from Your Experts?
The process of getting assistance with the DNP SOAP note from our nursing professionals is simple. The first step is sharing relevant patient case details and institutional specifications with our expert Consultants through our email. In the second step, we review the requirements and determine the extent of work to give a quote. Thirdly, our professionals begin the write up after we receive the payment. The fourth and final step involves delivering a high-quality SOAP note that is ready for submission. Review our order process to learn how to place an order with us.
